 
These are predominantly due to marked muscularis mucosae hypertrophy, which is also in part responsible for the lead pipe sign.Ĭolorectal carcinoma is often sessile. Strictures are also common and are not all malignant. Also in this region, extramural deposition of fat leads to thickening of the perirectal fat and widening of the presacral space 1,2. In chronic cases, submucosal fat deposition is seen, particularly in the rectum ( fat halo sign). In areas of mucosal denudation, abnormal thinning of the bowel may also be evident 2.Ī cross-section of the inflamed and thickened bowel has a target appearance due to concentric rings of varying attenuation, also known as mural stratification 1,2. 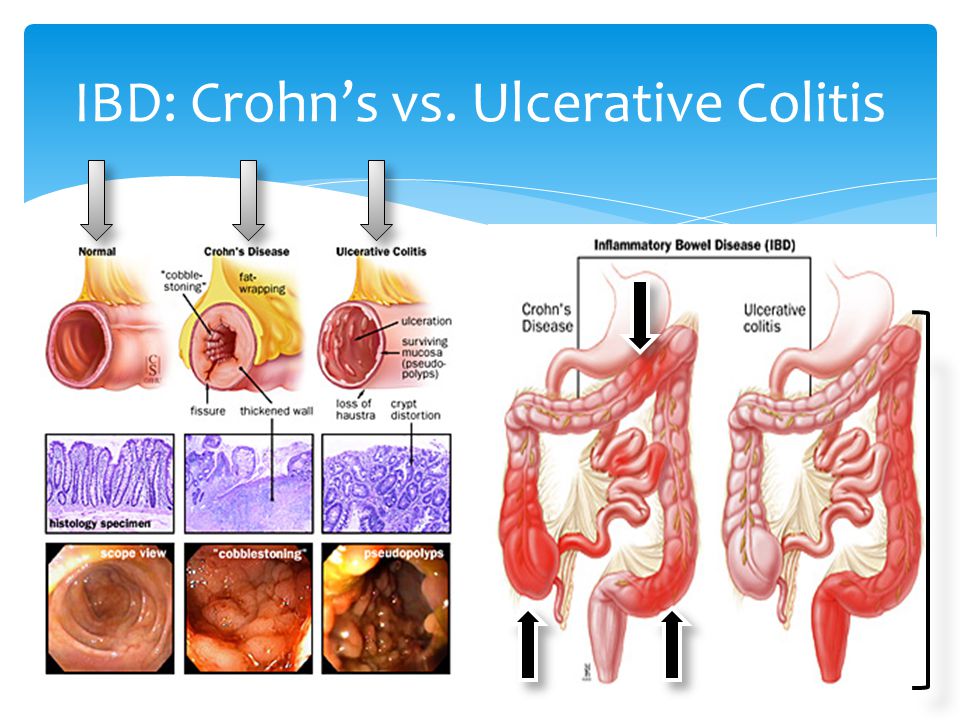
Inflammatory pseudopolyps may be seen if large enough, in well-distended bowel. 
It is important to note however that CT is insensitive to early mucosal disease 2. 
CTĬT will reflect the same changes that are seen with a barium enema, with the additional advantage of being able to directly visualize the colonic wall, the terminal ileum and identify extra-colonic complications, such as perforation or abscess formation. Small islands of residual mucosa can grow into thin worm-like structures (so-called filiform polyps)Ĭolorectal carcinoma in the setting of ulcerative colitis is more frequently sessile and may appear to be a simple stricture. In chronic cases, the bowel becomes featureless with the loss of normal haustral markings, luminal narrowing, and bowel shortening ( lead pipe sign). When most of the mucosa has been lost, islands of mucosa remain giving it a pseudopolyp appearance. Mucosal ulcers are undermined ( button-shaped ulcers). As inflammation increases, the bowel wall and haustra thicken. Mucosal inflammation leads to a granular appearance on the surface of the bowel. It is however contraindicated if acute severe colitis is present due to the risk of perforation. Fluoroscopyĭouble-contrast barium enema allows for exquisite detail of the colonic mucosa and also allows the bowel proximal to strictures to be assessed. Non-specific findings, but may show evidence of mural thickening (more common), with thumbprinting also seen in more severe cases. This leads to toxic megacolon, which although uncommon, has a poor prognosis 13. In very severe cases, the colon becomes atonic, with marked dilatation, worsened by bacterial overgrowth. The entire colon may be involved, in which case edema of the terminal ileum may also be present (so-called backwash ileitis). Involvement of the rectum is almost always present (95%) 1, with the disease involving variable amounts of the most proximal colon, in continuity. In this system,Įrosions and ulcers are characterized from 1-4 Ulcerative Colitis Endoscopic Index of Severity (UCEIS)Ī newer endoscopic scoring system which includes assessment of vascular pattern, bleeding, and ulcers and excludes mucosal friability. Total score ranges from 0-12 8.ġ: mild disease with evidence of mild friability, reduced vascular pattern, and mucosal erythemaĢ: moderate disease with friability, erosions, complete loss of vascular pattern, and significant erythema It is a composite of subscores from four categories, namely stool frequency, rectal bleeding, findings of flexible proctosigmoidoscopy/colonoscopy and physician’s global assessment. One of the most commonly used scoring systems. Thoracic manifestations of ulcerative colitisĮrythema nodosum and pyoderma gangrenosum Associationsħ0-80% of patients with PSC develop inflammatory bowel disease The diagnosis is often made with endoscopy, which also allows biopsy of any suspicious areas. Unlike Crohn disease which is characteristically a transmural disease, ulcerative colitis is usually limited to the mucosa and submucosa 5. PathologyĪ combination of environmental and genetic factors are thought to play a role in the pathogenesis, although the condition remains idiopathic. C-reactive protein levels are usually normal 6. Clinical presentationĬlinically patients have chronic diarrhea (sometimes bloody) associated with tenesmus, pain, and fever 1. Ulcerative colitis is less prevalent in smokers than in non-smokers. Typically ulcerative colitis manifests in young adults (15-40 years of age) and is more prevalent in males but the onset of disease after age of 50 is also common 1,3,5. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
